People under the age of 30 are being offered an alternative to the Oxford-AstraZeneca vaccine after a review into a possible link with rare blood clots in adults.
The UK’s medicine regulator – the MHRA – says the benefits of the vaccine still outweigh the risks for the vast majority of people.
What’s the potential issue with the vaccine?
The regulator looked into the number of people in the UK who had developed rare blood clots after receiving the AstraZeneca vaccine.
It found that 79 people – two-thirds of them women – experienced the clots after receiving a first vaccine dose. Nineteen of them died.
More than 20 million AstraZeneca vaccines doses had been administered across the UK by the end of March.
The MHRA said about four people in a million developed the blood clots.
It said it had not been proven that the jab had caused the clots. Its head, Dr June Raine, said while the link was “firming up”, more evidence would be needed.
The benefits of the AstraZeneca vaccine outweigh the risks of the virus – hospitalisation and death – for the vast majority of people, she said. But for younger age groups it was more “finely balanced”.
What are these rare blood clots?
The MHRA study looked at people who had developed clots associated with a low level of platelets after receiving the Oxford-AstraZeneca vaccine.
Platelets are tiny blood cells that help your body form clots to stop bleeding.
Among these clots is a type called a Cerebral Venous Sinus Thrombosis (CSVT).
CVST occurs when a blood clot forms in large veins in the head – stopping blood from draining out of the brain.
As a result, blood cells may break and leak into brain tissue – ultimately leading to a stroke.
The clot can occur naturally,
CVST is considered a rare type of stroke and affects about five people in a million each year – according to Johns Hopkins School of Medicine.
They are more common, but still very rare, in younger women.
What symptoms should I watch out for?
The MHRA says anyone who has these symptoms four or more days after receiving the Oxford-AstraZeneca vaccine should seek prompt medical advice:
- A severe or persistent headache
- Blurred vision
- Chest pain
- Shortness of breath
- Swollen legs
- Persistent abdominal pain
- Unusual skin bruising
- Pinpoint spots (not including the injection site)
Covid infection itself can make clots more likely, stresses the MHRA.
What is the latest advice?
The MHRA is not recommending age restrictions regarding use of the AstraZeneca vaccine – but it says under-30s with no underlying health conditions should be offered an alternative vaccine where available.
This is because the data suggests there’s a slightly higher incidence of clots reported in younger adult age groups.
Based on the current data, the following is also advised:
- Anyone who experiences clotting after a first dose of the vaccine should not receive a second dose
- People with a history of blood disorders (at risk of clotting) should only have the AstraZeneca when the benefits outweigh the risks
- Pregnant women should talk to their GPs about the benefits and risks
A trial of the Oxford-AstraZeneca Covid vaccine on children had already stopped giving out jabs because of the MHRA review.
What have other countries said about the AstraZeneca vaccine?
The European Medicines Agency (EMA) has said clotting should be listed as a very rare vaccine side effect.
After a study looking at 86 such cases in the EU, the EMA concluded the benefits of the vaccine outweighed the risk. There was no definite causal link.
Germany has suspended the use of the vaccine in people under 60 as a result of CSVT cases recorded in the country.
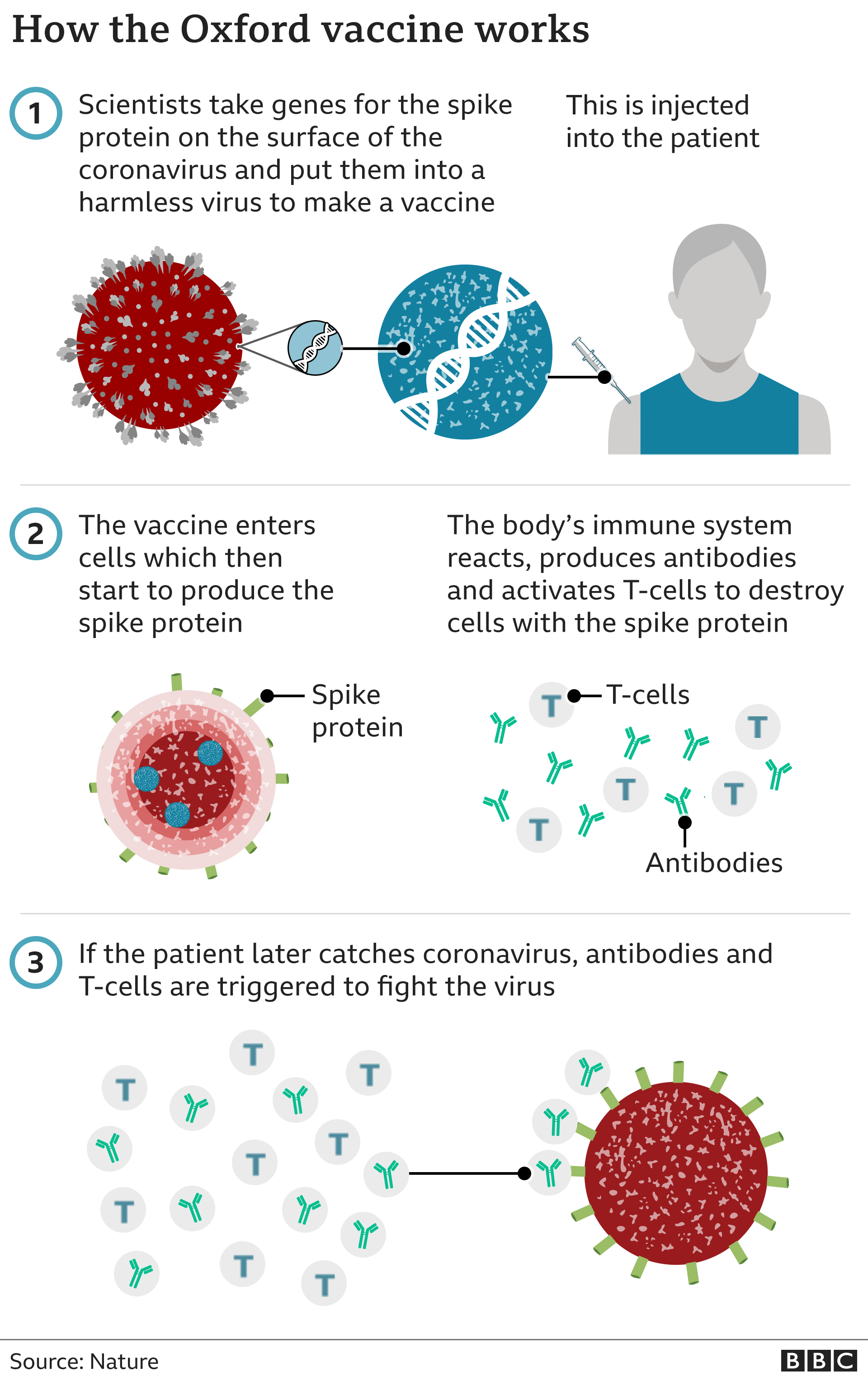
How does the Oxford-AstraZeneca vaccine work?
It is made from a weakened version of a common cold virus (known as an adenovirus) from chimpanzees. It has been modified to contain genetic material shared by the coronavirus – although it can’t cause the illness.
Once injected, it teaches the body’s immune system how to fight the real virus.
Is the Oxford AstraZeneca vaccine as good as the Pfizer?
Large trials showed the Pfizer vaccine was 95% effective, while the figure for the Oxford one was 62%.
But directly comparing results is difficult because there are differences in the way the trials were carried out.
No-one who received the Oxford vaccine was hospitalised or became seriously ill due to Covid.
A recent study found a single dose of the Oxford vaccine offered 76% protection for three months, and this went up to 82% after the second dose.
Does it work in older people?
Some European countries initially offered the vaccine only to 18-64 year-olds because they said there was limited data on how well it protects the over-65s.
The EMA approved the vaccine in January for use in all age groups, including older adults.
How long do vaccines protect against Covid?
It is not yet known how long protection lasts with any of the coronavirus vaccines.
A study found that unvaccinated people who have had Covid, develop protection for at least six months. Vaccines are likely to provide stronger protection than this.
It may be that people need annual vaccinations, as happens with the flu jab.
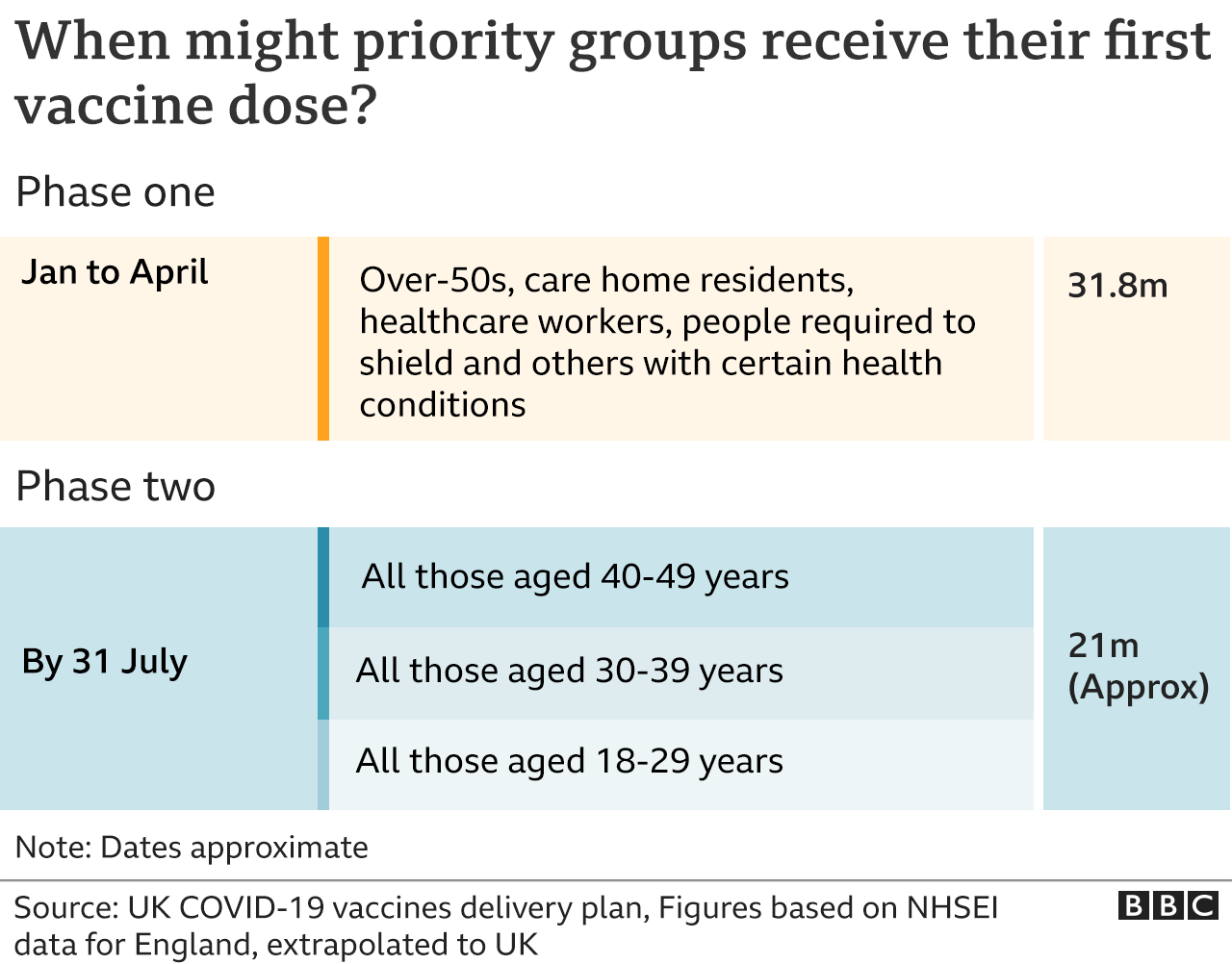
Does the vaccine protect against new variants?
Experts are studying all of the current coronavirus vaccines to check how well they work against new, mutated variants of the virus.
The government’s deputy chief medical officer, Jonathan Van Tam, says there is “plenty of evidence” the vaccines appear to be effective against the Kent variant which is dominant in the UK.
There is less evidence about protection for other ones, such as the Brazil and the South Africa variants.
A study based on about 2,000 people suggests the Oxford-AstraZeneca vaccine offers limited protection against mild and moderate disease caused by the South Africa variant.
However, there is no evidence to suggest it would not be effective at preventing more severe cases that need hospital treatment.

